Radiotherapy for breast cancer
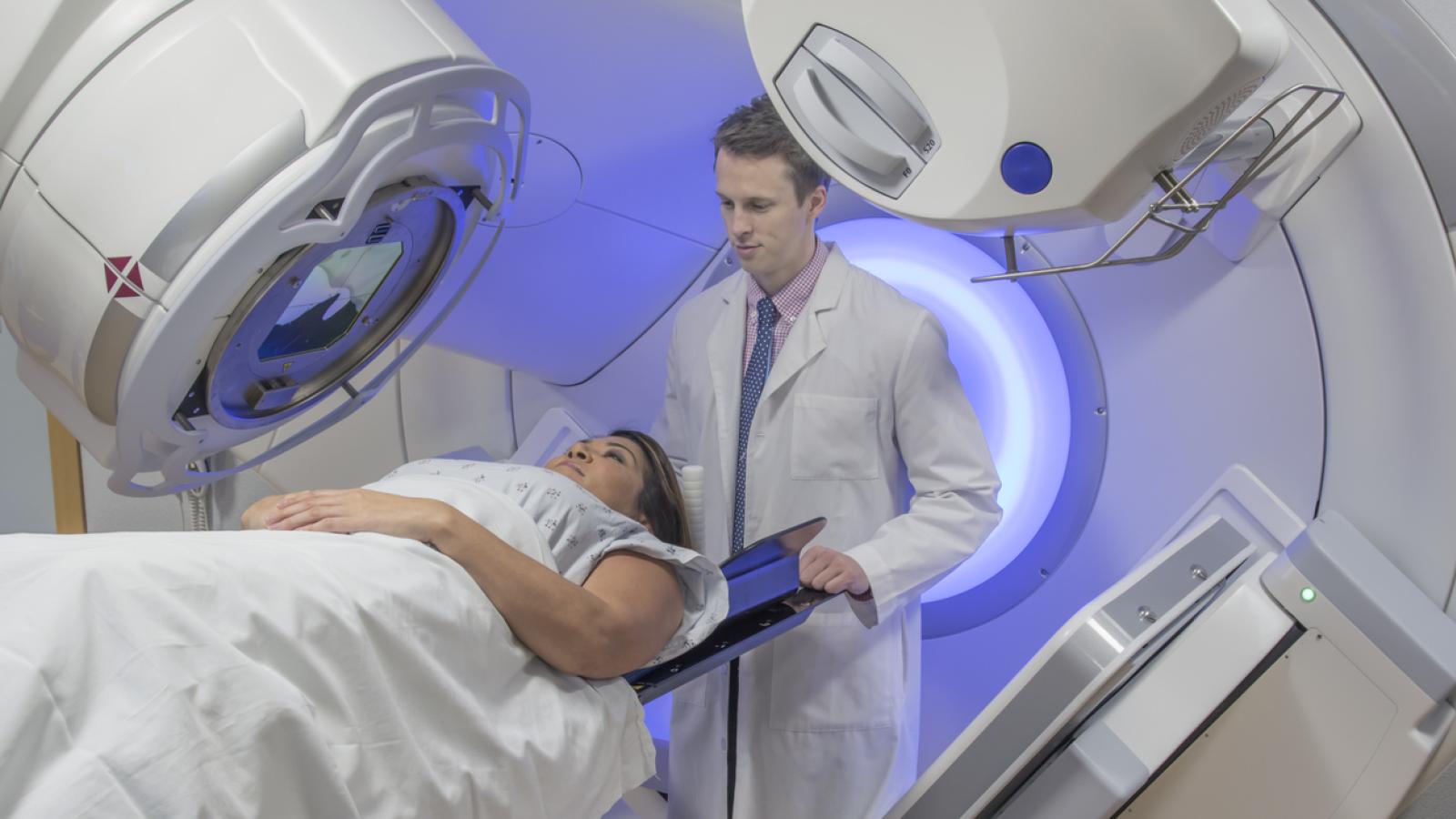
Two types of radiotherapy can be used for breast cancer:
You might have both internal and external radiotherapy.
Why might I have radiotherapy?
Radiotherapy for breast cancer may be given:
After surgery (in the area where the tumour was) to reduce the risk of the cancer coming back.
Radiotherapy may be recommended if your lymph nodes contained cancer. If your tumour was large, you might have radiotherapy to the chest wall area.
With chemotherapy to help the treatment work better.
To relieve symptoms such as pain, if the cancer is advanced or has come back. This is called palliative radiotherapy.
If you are planning breast reconstruction, external radiotherapy to the breast may affect the type of breast reconstruction you can have. Your doctor and breast care nurse will give you further information.
External beam radiotherapy
High-energy rays are aimed directly at your cancer cells to destroy them. The radiation only affects the cells in the treated area.
Planning
You will need to go to hospital before your treatment for at least one radiotherapy planning session. This involves a CT scan to plan the treatment accurately in the tumour area. Tiny tattoo dots are placed on your skin to help get you into the exact same position for each treatment.
Getting treatment
Each treatment only takes a few minutes. You will lie on a bed and be positioned using the tiny dots on your skin as a guide. A machine called a linear accelerator will deliver the beams of radiation to the right place. The machine will move around you but does not touch you. Radiotherapy doesn’t hurt, but you might be a bit uncomfortable from holding your arm in the same position.
You won't be radioactive after your treatment, so you can be around other people safely.
Raising your arm
Before treatment, you should be able to raise your elbow to at least shoulder level so that you are comfortable in your treatment position. If you find this difficult, ask to see a physiotherapist before starting treatment.
If you are on pain medication after surgery, take your painkillers before you go to your appointment.
How much treatment will I need?
Your doctor will let you know how many sessions or treatments you need. Usually you come into hospital for treatment every weekday for a number of weeks. Treatment given after surgery may take as little as 1 week or last up to 4 weeks.
For radiotherapy to relieve symptoms like pain (palliative radiotherapy), you usually have only one or a few treatments.
Side-effects of breast radiotherapy
Everyone is different, so it's hard to predict if you will get any side-effects and if so, which ones. If you do get any side-effects they usually develop during or shortly after your treatment and get better within a few weeks.
Short-term possible side-effects
- Skin changes / irritation at the treated area (for example nipple soreness, changes to the appearance of the skin or flaking, peeling skin). If the skin breaks down, tell your nurse or radiation therapist so they can protect it with a dressing.
- Tiredness (fatigue)
- Indigestion
Possible late side-effects
Late side-effects may develop some time after treatment. Some side-effects last a long time or may even be permanent.
- Changes to the colour or feel of the breast. For example, more obvious thread veins in the treated area or hardening of the breast tissue.
- Muscle tightness and loss of movement in the chest or shoulder area
- Lymphoedema – swelling caused by a build-up of lymph fluid
- Breast swelling and pain, which can last up to a year after radiotherapy
- Nerves damage, which can cause tingling, numbness, pain, weakness and possibly some loss of movement in your arm
- A dry cough, shortness of breath caused by fibrosis in your lung. This isn't common
- You probably won’t be able to breastfeed your baby on your treated breast
- Some people can have damage to the heart after radiotherapy to the left breast but this is very rare
Breast swelling and pain can happen for up to a year after radiotherapy. Other side-effects can happen months or even years after treatment. Read more about radiotherapy side-effects and tips to help with them.

If you feel unwell or have any other side-effects or symptoms, during or at any time after treatment, tell your doctor, nurse or radiation therapist.
Internal radiotherapy (brachytherapy or interstitial radiotherapy)

(Image courtesy of CRUK / Wikimedia commmons)
Brachytherapy gives a high dose of radiation to a small area. It’s usually given after breast surgery.
Small radioactive pellets (implants) are put into your breast near where the tumour was removed and left for a few days or a few minutes, depending on the dose of radiation. Most people have up to 10 treatments.
The pellets are put in through small tubes (catheters) called applicators, which are put into your breast under local or general anaesthetic. You will have a CT scan to check the tubes are in the right place.
The applicators will be removed after you have finished treatment. You will need to stay in hospital during treatment.
You may have brachytherapy instead of external radiotherapy or you may have both.
Your medical team will talk to you about this treatment in greater detail if it is recommended for you.
For more information
Phone
1800 200 700



