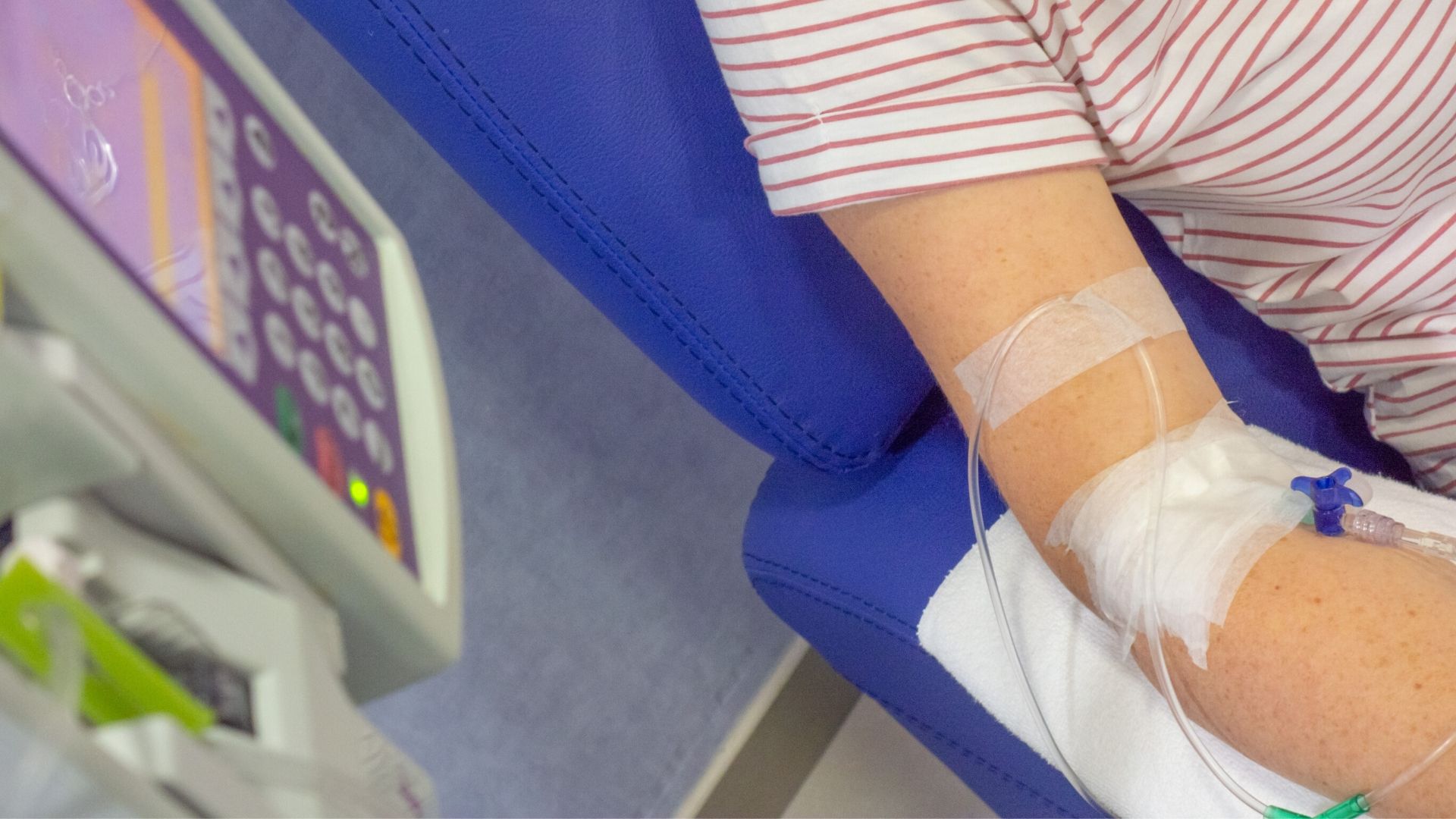
Chemotherapy for AML
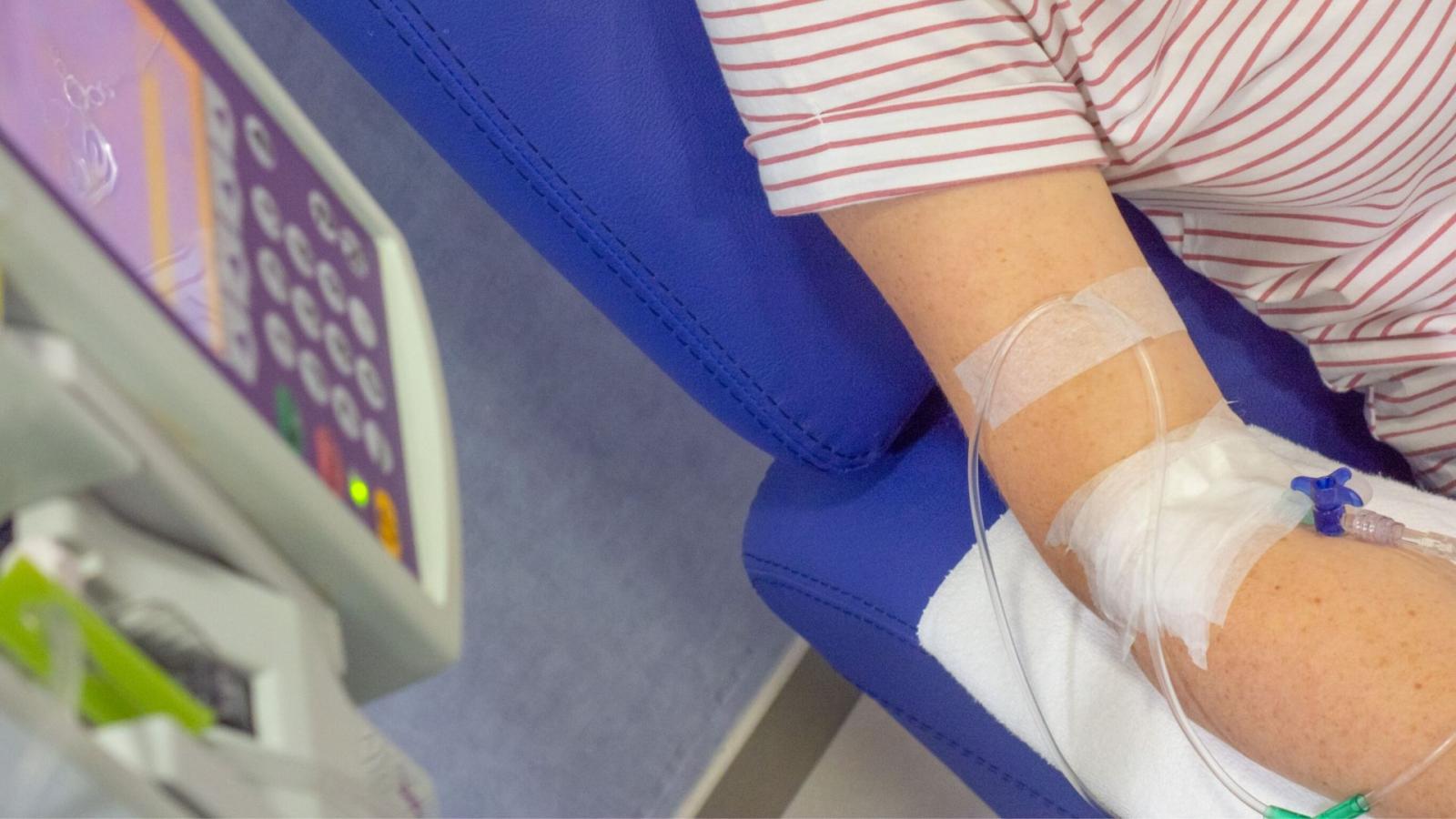
On this page:
Chemotherapy uses drugs to kill cancer cells. There are two main stages of chemotherapy for AML:
Induction
An intense dosing of chemotherapy, which aims to get rid of all the leukaemia from your blood and bone marrow and quickly get your bone marrow working normally again (remission). This stage is called induction chemotherapy or remission induction.
Induction usually involves two cycles of a combination of chemotherapy drugs. When the induction is over, a bone marrow test will be done to check if the leukaemia has gone into remission.
Remission is when your bone marrow is producing blood cells normally and you have fewer than 5% of the immature leukaemia cells in your bone marrow. If your remission lasts indefinitely, you are said to be cured.
Consolidation
The aim of this phase is to reduce the risk of relapse once you are in remission. You will usually need 2-3 more cycles to complete the consolidation phase of treatment, but this can vary depending on the type of AML you have and the progress of the disease. Without these cycles, there is a higher risk of your leukaemia coming back in the first year. You might also have a stem cell transplant.
If you do have a transplant, you might not have any further chemotherapy, or you might just have one more course.
Read more about chemotherapy and its side-effects.
How long does AML chemotherapy treatment last?
Intensive chemotherapy usually involves 3 or 4 courses or blocks of treatment over a 4-6 month period. Each course lasts a number of days and it usually takes your blood count 3-4 weeks to recover. You’ll have most of your treatment as an inpatient in hospital, but nearly all patients will get to go home for a week or so between courses.
Non-intensive treatment
Non-intensive treatment involves low doses of chemotherapy or other drug treatments, for example, targeted therapies. Non-intensive treatment can be less effective in guaranteeing long-term remission, but it is easier on your body. This may be a better option if you are older or have other medical problems. Azacitidine (Vidaza®) is an example of a drug used for non-intensive treatment. There are lots of different options for non-intensive treatment. Your treatment, and the way it is given, will be tailored to your individual disease type and needs.
Side-effects
The side-effects of intensive chemotherapy can be hard on your body, but they normally go once treatment is over. You are likely to have side-effects related to reduced levels of blood cells such as anaemia (low red blood cells), increased risk of infection (low white blood cells) and bruising and bleeding (low platelets). Your doctor or nurse will discuss any possible side-effects with you before your treatment.
Remember, contact your doctor or hospital without delay if you think you have an infection. Sepsis (blood poisoning) can develop as the body reacts to an infection.
For more information
Phone
1800 200 700