How is anal cancer treated?
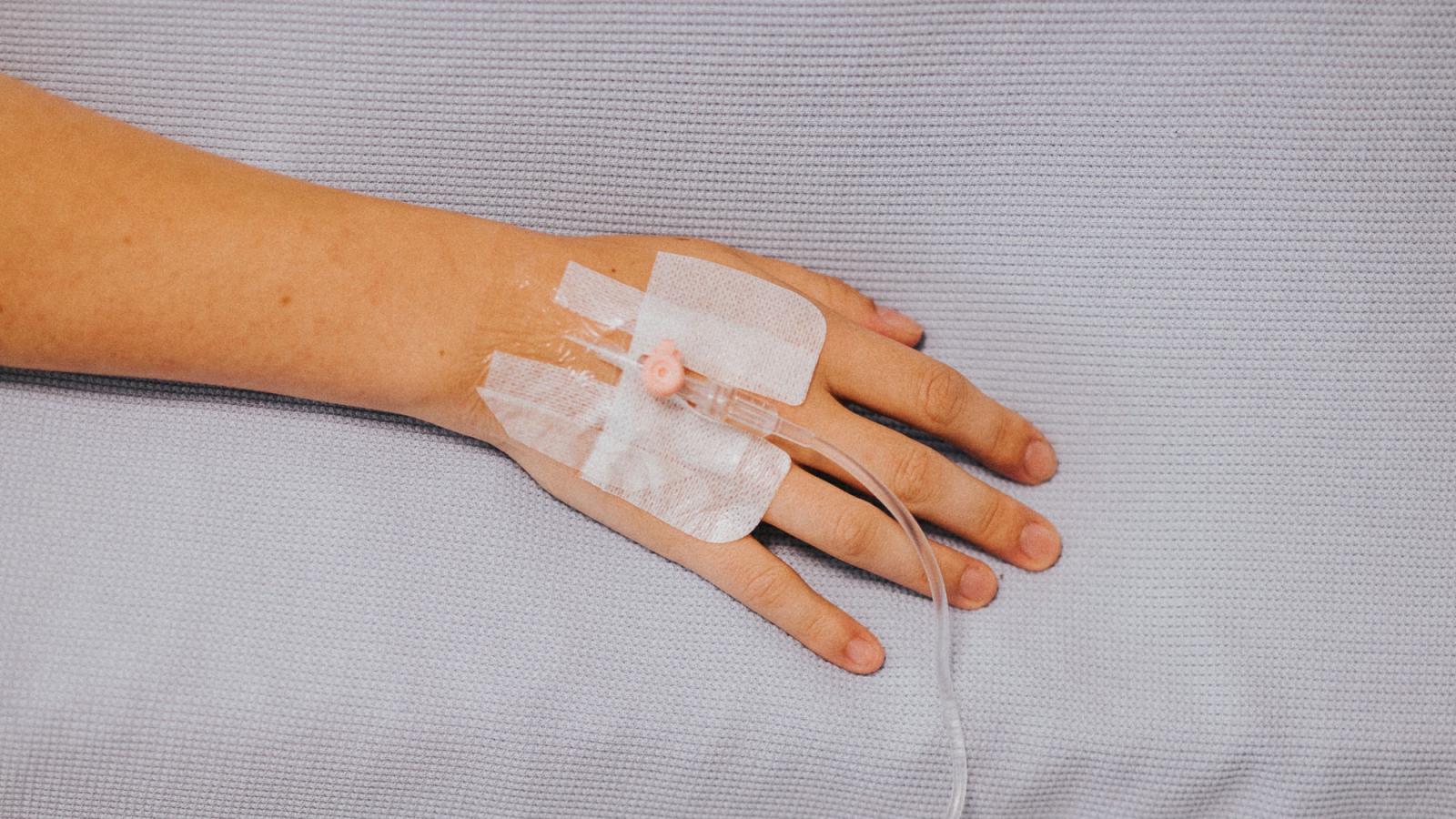
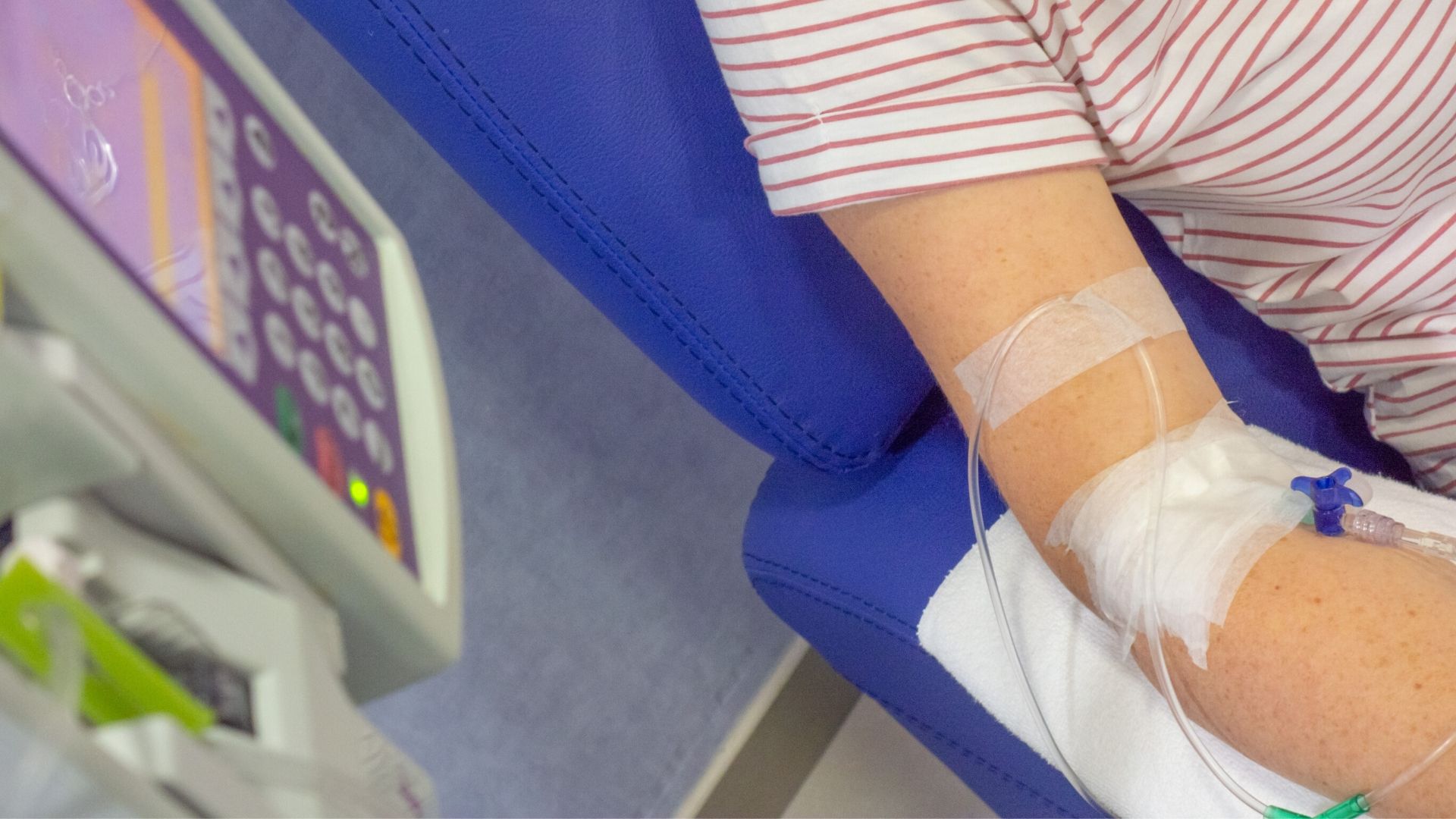
Chemoradiation (chemotherapy and radiotherapy together)
Doctors often use a combination of chemotherapy and radiotherapy to treat anal cancer. This is called chemoradiation.
This combination treatment is usually very successful.
Chemotherapy
Chemotherapy is a treatment using drugs to cure or control cancers. The drugs can be taken in tablet form or injected into a vein.
Chemotherapy can be used in different situations to treat anal cancer. It is often given with radiotherapy. Read more about chemotherapy.
Radiotherapy
Radiotherapy uses high-energy X-rays to kill the cancer cells in your anus. These rays are aimed directly at the cancer cells to destroy them while doing the least damage to normal cells. It's often given for 4 to 6 weeks.
Often you'll have both radiotherapy and chemotherapy. Read more about radiotherapy.
Surgery
If your cancer is not fully gone after chemoradiation, you may need some surgery. The type of surgery will depend on your cancer and your doctor will discuss it with you in more detail.
There are two main types of surgery:
Local resection: This surgery is used for small tumours. It only removes the area where the cancer cells are found.
Abdominoperineal resection: This is where your anus and rectum are removed. Having this surgery means that you will have a permanent colostomy.
A colostomy is where your bowel opens onto the surface of your abdomen through a cut in your skin called a stoma. A bag is placed over this opening to collect your stool.
You can speak with a specialist stoma nurse if you need this type of surgery. We also have information on caring for a stoma.
Will I get side-effects?
The type of side-effects you get will depend on the type of treatment, the dose, the duration and your own general health.
If you have chemoradiation you may get both chemotherapy and radiotherapy side-effects, which can be more severe than just having one treatment.
Ask your doctor or nurse about any possible side-effects before your treatment starts.
Read about the different treatments to find out more about possible side-effects.
We also have information to help you cope with different side-effects and symptoms.
Treating metastatic cancer
Metastatic anal cancer means the cancer has spread beyond the anus to other parts of the body. Not all cancers spread.
If you have metastatic cancer, your doctor will aim to slow down the growth of the cancer and reduce or relieve any symptoms you have.
Treatment includes surgery, chemotherapy and radiotherapy. Or you may be suitable for a clinical trial.
Read more about metastatic cancer.
For more information
Phone
1800 200 700