Radiotherapy
Radiotherapy is the use of high-energy radiation to kill cancer cells.
What is radiotherapy?
Radiotherapy uses high-energy radiation to kill cancer cells.
Why might I have radiotherapy?
- To cure your cancer
- To shrink a tumour before surgery, to make it easier to remove
- To kill any cancer cells that remain after surgery
- To stop cancer spreading
- To treat cancer that has come back after treatment
Palliative radiotherapy
You might have radiotherapy to help with symptoms like pressure, pain or bleeding or to slow down the cancer’s growth. This is called palliative radiotherapy. Often a short course, sometimes only a single treatment, is needed.
How does radiotherapy work?
Radiotherapy damages the cancer cells’ DNA. This will stop the cancer cells from dividing and growing.
Radiotherapy and other cancer treatments
Radiotherapy can be given in combination with other treatments, such as surgery, chemotherapy, hormone therapy and targeted therapies. For some cancer patients, radiotherapy is the only treatment needed.
Chemoradiation
Taking certain chemotherapy drugs can make the cancer cells more sensitive to radiation (radiosensitisers). This helps the radiotherapy to work better. Having chemotherapy and radiotherapy together is called chemoradiation.
Will I get side-effects?
If you get any side-effects they mostly affect the area being treated. For example, diarrhoea or constipation after stomach / pelvis radiotherapy, a cough after chest radiotherapy. Most side-effects ease in the weeks and months after treatment.
Usually you don’t get side-effects with palliative radiotherapy. We have more information on radiotherapy side-effects.
Where will I have radiotherapy?
You can get radiotherapy in special cancer treatment centres. The radiotherapy unit may be in a different department or a different hospital from where you have been before.
Coping with radiotherapy
Radiotherapy treatment can be tiring, as you usually have to go to hospital 5 days a week for a number of weeks. This can be even harder if you have to travel some distance to get treatment. Sometimes it may affect your ability to work or look after your family.
Get help with travel
- Ask friends and family to help with travel, if you find it tiring
- Ask your radiation therapist or medical social worker at the hospital for advice if you need help with travel
- Our Travel2Care scheme may be able to help with travel expenses
Staying overnight
- It may be possible to stay at the hospital in guest accommodation. Your cancer specialist may have to write a letter requesting this service for you.
- If you need advice about nearby B&Bs or hotels, the radiotherapy staff may be able to give you some advice.
Work
- Some people find that they can carry on as normal during treatment and continue working. Others might find it very tiring and prefer to stay at home and take sick leave from work or school or college. Read more about work and cancer.
- Don’t be afraid to ask for help if you feel overwhelmed, especially if you have young children or older parents to care for.
Side-effects
- Talk to your medical team if you’re bothered by any side-effects. Don’t suffer in silence! We have more information on coping with side-effects and symptoms.
Types of radiotherapy
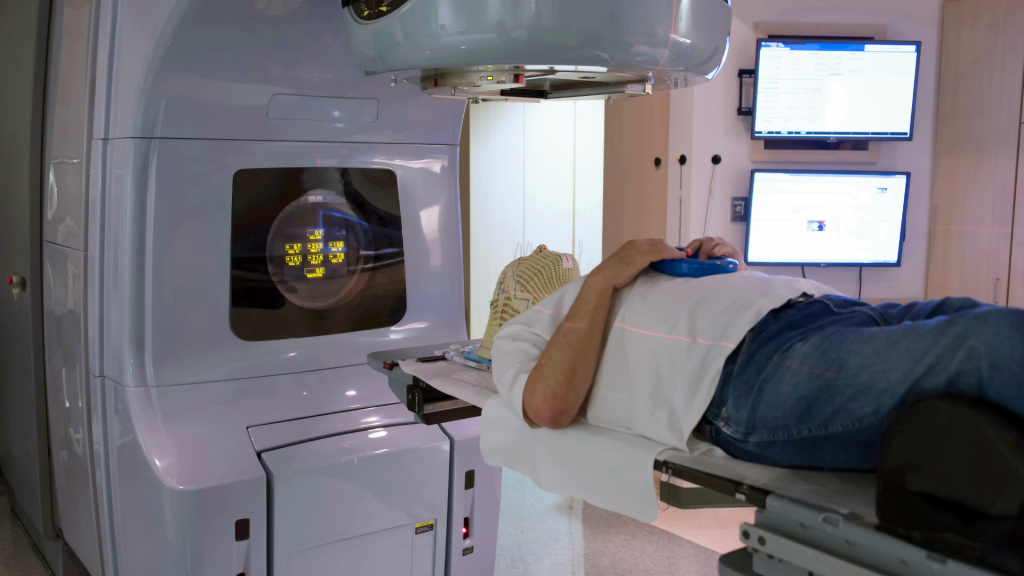
External beam radiotherapy
This is the most common type. Beams of radiation are aimed into your tumour (or the tumour site if you have already had surgery to remove the tumour). The beams come from a machine called a linear accelerator. You will have to go for planning sessions beforehand if you’re having external radiotherapy. This is to plan the dose of radiotherapy you will need and mark out the exact area that needs to be treated.
Read more about external radiotherapy.
Internal radiotherapy (brachytherapy)
Here a radioactive material is put inside your body to kill the cancer cells. Brachytherapy is used for treating cancers such as prostate, oesophageal and head and neck cancers.
Read more about internal radiotherapy.
Systemic radiotherapy
Liquid radioactive drugs called radionuclides or radioisotopes are given by mouth or put into a vein to treat certain types of cancer like thyroid and advanced (metastatic) prostate cancer. These drugs travel throughout the body and they find and destroy cancer cells.
You may have both internal and external radiotherapy.

Radiotherapy content reviewed by Dr Dayle Hacking, Consultant Radiation Oncologist and Loretto Gallagher, Clinical Nurse Specialist in Radiation Oncology. Oct 2022
For more information
Phone
1800 200 700