Stem cell transplants using another person’s stem cells (allogeneic transplants)

An allogeneic (donor) stem cell transplant allows you to have higher doses of chemotherapy and/or radiation therapy to destroy your bone marrow and replaces your bone marrow that is no longer working properly with healthy stem cells from your donor. Your donor may be a family member or an unrelated donor.
There are 5 main stages:
- Preparing for the transplant: You have tests to check your general health, and are given advice on preparing for the treatment. Doctors will look for a donor whose cells match yours.
- High-dose (conditioning) treatment: You have a combination of drugs including chemotherapy and/or radiation and drugs to suppress your immune system to destroy your bone marrow and immune system. This prepares your body to accept your donor’s cells.
- Having the transplant: You are given your donor’s stem cells through a drip.
- Waiting for new blood cells to grow: Your donor’s stem cells find their way to your bone marrow and start to grow and make healthy new blood cells. This is called engraftment. You will be looked after in isolation and you will need lots of medical and nursing support at this time.
- Recovering after the transplant: When your blood cells have recovered and you are well enough, you can go home. Your doctor or nurse will give you advice about avoiding infection. You will have regular follow-up appointments at the hospital to check your recovery.
Preparing for a donor (allogeneic) stem cell transplant
Tests
- Blood tests: Blood tests can show the numbers of different types of blood cells. This is called a full blood count. Doctors will also check your blood group, clotting and iron levels and how well your kidneys, liver and bones work. They will also check for the presence of viruses, for example, HIV, hepatitis A, B, C and syphilis.
- 24-hour urine collection: This test checks how well your kidneys are working. You will be given a large plastic bottle to bring home with you to collect your urine. You will be asked to collect all the urine you pass in a 24-hour period. You do this at home. It is important to collect all the urine you pass in the bottle or the test will have to be repeated. To measure the results, you will need a blood test taken when you return the urine collection to the hospital.
- Dental check-up: Before you have the high-dose chemotherapy, a dentist needs to check your teeth. This is because decaying teeth can cause a serious infection during treatment. You can visit your own dentist for this check-up. Your doctors will need a letter from your dentist saying that you are dentally fit for the transplant
- Testing for bacteria: Certain bacteria which are not usually harmful may cause infection after high-dose chemotherapy. Tests will help your doctor choose the correct antibiotics if you do become unwell.
- Lung function tests
- Chest X-ray
- Heart tests (ECG and echocardiogram (ECHO)
You may have other tests, depending on your condition and medical history. For example, bone marrow biopsy and lumbar puncture. Read more about cancer tests.
Having a central line put in
Before your high-dose chemotherapy, you will need a special line (tube) placed in a large vein. Any treatment or medication that needs to go into your veins can be delivered through the line, meaning there is no need for needles in your arms every time. It can stay in place during and for a time after your treatment. Read more about central lines.
Treatment (chemotherapy)
You may have chemotherapy before your stem cell collection, to reduce the number of cancer cells.
Life and work
You can expect to be in hospital for about 6 weeks. If you live more than an hour from the transplant centre, you will need to stay in the Dublin area for about another 6 weeks. Before treatment you may want to:
- Organise your finances, including any social welfare benefits you may be entitled to
- Talk to your employer about sick leave
- Organise childcare
- Organise a family member or carer to stay with you for 6 weeks after you leave hospital
- Ask a close friend or family member to provide updates to everyone else
The medical social worker in your hospital will be able to help and advise you about some of these issues.
Fertility
High dose treatment can affect your ability to have children in the future. Talk to your medical team before treatment if this is important to you. It may be possible to freeze your eggs or sperm.
Finding a donor
Doctors use your tissue type to match you with a donor. Your tissue type is the combination of proteins called human leukocyte antigen (HLA) markers on the surface of your cells. You will have a blood test to find your tissue type. There are different types of donors:
- Sibling: a brother or sister. If you have a brother or sister are most likely to have a good match for your tissue type, so they will be tested first.
- Alternative family donor: a parent, cousin or child
- MUD: a volunteer Matched Unrelated Donor
All donors will need tests such as blood tests and a chest X-ray to make sure that they are fit and healthy.
Having the best possible match means less risk of:
- Your body rejecting the new stem cells
- The new immune cells reacting against your other body cells.
High-dose treatment
Before you have your transplant, you will have high doses of chemotherapy or radiotherapy, or a combination of the two. You may also have drugs that will work on your immune system. This is called conditioning treatment.
Not all patients have radiotherapy. Your transplant team will give you more information on radiotherapy if this is part of your treatment.
Almost all patients have chemotherapy. This can either be given in tablet form or into your vein (intravenously). Intravenous chemotherapy is given through your central line, infused over an hour or a number of hours. It can also be given by injection.
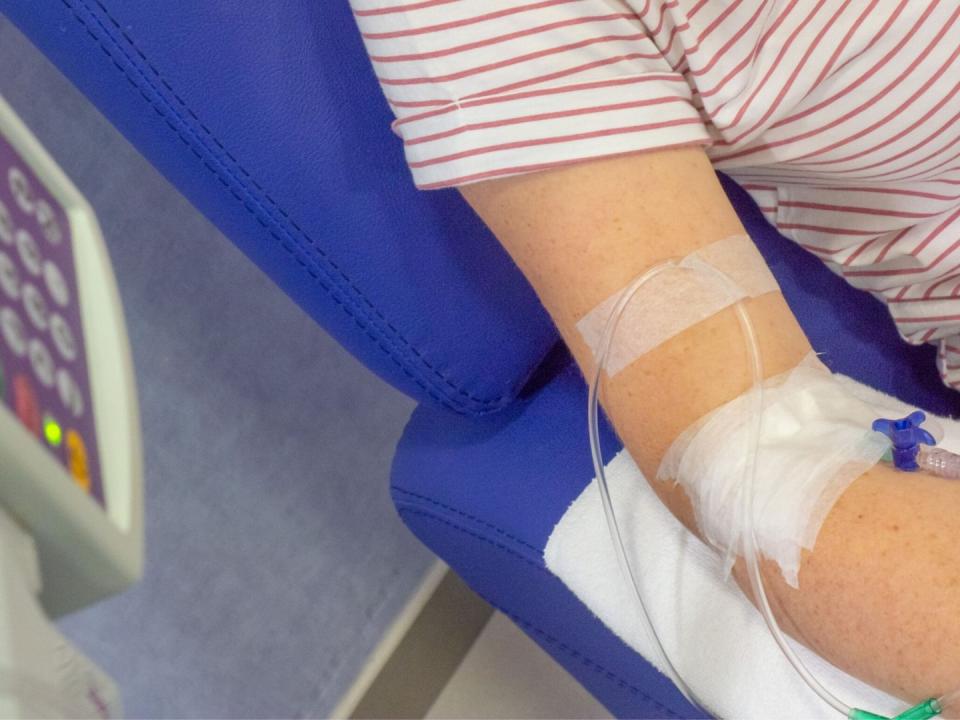
You usually begin conditioning treatment the day after you go into hospital. It can take anything from 5 to 12 days.
The high-dose chemotherapy will cause your blood count to fall. In particular, your white blood cells will be very low. This means your immune system will be less strong and you will be at risk of infection. You are likely to experience some side-effects of chemotherapy. Read more about side-effects.
Receiving the donor stem cells
Most patients have their transplant the day after they finish conditioning treatment. But this can vary depending on the treatment and the type of transplant.
The cells are infused through your central line into your bloodstream.
The actual infusion of the donor cells can seem a little bit of an anti-climax as it is just like having a blood transfusion. The length of time for the infusion depends on how the stem cells are collected from your donor:
- Directly from the bone marrow: Bone marrow cells are given fresh and usually take two to four hours to infuse
- From the blood (peripheral blood stem cell harvest): You may have the collected cells infused in one session, or you may receive one bag on the first day of collection and one on the second. Each bag usually takes about 30 minutes to infuse.
The day you receive the stem cells is known as Day 0 (zero). This is because the staff measure your recovery starting from this day.

After getting the stem cells
If the stem cells were frozen before being infused you may notice a strange taste and smell after the infusion. The smell is like garlic or boiled sweetcorn. This is due to DMSO, which is a preservative used to protect the cells while in storage. It is nothing to worry about and the smell and taste will clear within a day or two.
Waiting for new blood cells to grow (engraftment)
Your donor’s stem cells will travel through your blood to your bone marrow, where they will start to grow and mature into new blood cells. This is called engraftment. You will need blood and platelet transfusions until you begin to produce your new blood cells.
Engraftment happens over 2 to 3 weeks, but can sometimes take longer. The first sign is often a rise in your white blood cell count. This rise can sometimes be unsteady, so don’t worry if your count goes up and down a little at the start.
You may be given a drug called a growth factor as an injection. This will boost the growth of the stem cells and help them mature. The number of white blood cells (your neutrophils) will be very low for some time. This is called being neutropenic. Neutrophils are very important in fighting infection. Your transplant team will try to protect you from possible infection during this time.
Avoiding infection
You will be looked after in a single room. The room will have a special air conditioning system to keep the air in your room very clean. You will be closely watched and checked for signs of infection.
Visitors
It is best that only your close family and friends visit you during your stay. This is to reduce the chance of you and other patients picking up an infection. The best advice is that no more than two people visit you at any one time.
Coping with isolation
Being in isolation after the transplant can be stressful. Naturally you might find it difficult being on your own without other patients around you. Your nurses can help you overcome these difficulties and will make your stay as non-traumatic as possible. They can arrange for you to talk to a clinical psychologist to explore your feelings and try to help you cope.
Moving around
Keeping active helps to keep your muscles working and is important for your lungs. Get up and walk around the room at least a few times a day. Even getting up to go to the toilet and to wash yourself helps with your recovery. You will be allowed to exercise and the occupational therapist or physiotherapist may plan an activity programme for you. You may be allowed out of the room for short periods when your blood count has started to rise.

Side-effects
You are likely to experience some side-effects from your stem cell transplant. Tell your medical team about your side-effects or if you feel unwell in any way. It's helpful to learn about potential side-effects in advance so that you can be prepared.
Find out about stem cell transplant side-effects
Going home
You may feel excited, but you may also feel anxious about leaving behind the care you received in hospital. Talk to the nurses about any worries you have before you leave the hospital. If you have any questions after you go home, you can always call the transplant unit.
Things to look out for at home
You need to contact the hospital immediately if you develop any of the symptoms listed below or if you if feel unwell in any way. It is very common for patients to be re-admitted to hospital in the weeks or months following discharge. Try not to feel worried or disappointed if this happens to you.
Central line
- Shivering episode after flushing your line
- Swelling, tenderness or pus around your line
Bowels
- Persistent diarrhoea or constipation
- Change in the colour or consistency of your stools (poo)
- Cramps
Urine
- Change in colour
- Pain or burning sensation
- Red urine, clots or difficulty passing urine
Skin
- Any kind of a rash
- Itching
Temperature/shivering
- Temperature over 38ºC, with or without shivering
- Shivering with or without a temperature
Pain
- A persistent headache that does not respond to paracetamol
- Stomach ache
- Gut cramps
- Joint pain
- Mouth ulcers or a sore throat
Nausea or vomiting
- Let the hospital know if this is new or is preventing you from drinking or taking your medication.
Medicine
- Let the hospital know if you’re unable to take your medication for any reason.
Bleeding
- Any signs of bleeding or bruising. For example bleeding gums, or blood in the urine or stools (poo)
- Persistent nosebleed
Cough or breathlessness
- A new or persistent or worsening cough
- Shortness of breath or increasing shortness of breath
Check-ups
For the first few weeks after your transplant you need regular check-ups, often daily at first. This is called follow-up. You might need regular blood or platelet transfusions. Once your blood counts are stable and your strength is improving, you will have fewer appointments. Your doctor will decide how often you need to be seen.
It is likely that you will need follow-up appointments for a long time after your transplant. This will depend very much on your original disease but you may need blood tests, bone marrow tests or scans.
Central line
Your central line can usually stay in until your blood counts are high enough to allow it to be removed. If the line needs to stay in place, you or a family member will be shown how to care for it at home. It will also need to be cared for weekly with a flush and dressing change on the day unit.
Medications
You will have medications to take at home. Some of the common ones are:
- Anti-sickness medication, but you may not experience nausea or vomiting at all
- Antacid – to treat heartburn
- Antibiotics to protect against a particular strain of pneumonia
- Anti-viral drugs to protect against the cold sore and shingles virus
Continue to take any medications you are given until your doctor decides to stop them.
Tiredness (fatigue)
For the first few weeks after the transplant your energy levels will be very low. Fatigue can be a frequent and unpleasant side-effect. You will probably find you have no energy and do not feel like doing anything at first. Just getting up, washed and dressed can be a challenge in the first few weeks. Don’t expect too much from yourself – take one day at a time. This tiredness can last for a few months but sometimes can take longer to overcome. Read more about coping with fatigue.
Avoiding infection
Even if your blood counts are back to normal, your immune system takes a little longer to recover. Continue to be careful. For example:
- Continue to shower every day and be strict about your personal hygiene.
- Continue your mouthwashes until your next visit to the day ward.
- Avoid people with infections.
- Avoid areas that are overcrowded.
- Avoid close contact with pets, especially birds, in the first few weeks.
- Avoid swimming if you go home with your central line in place.
- Keep your fridge clean.
Appetite and diet
You may find that you don’t have much appetite or your taste and sense of smell has changed. Foods that you loved before might now begin to taste and smell different. Try not to worry as your appetite and taste will gradually improve. It’s important to eat as well as you can, so ask to talk to the hospital dietitian if you’re experiencing problems or losing weight. We also have advice on eating difficulties, including tips to help if your appetite is poor.
Aim to drink 2 to 3 litres of fluid a day to speed up your recovery. Your mouth may continue to feel dry after your transplant so drinking plenty of fluids will also help with this. Often it is best to avoid alcohol for a time after your transplant. Talk to your doctor for more advice about alcohol.
Your sex life
It is likely that after your transplant your sex life will be affected in some way. Tiredness, anxiety and lack of interest can often be the reason. It is likely that once your energy levels return to normal so too will your sex drive (libido). If your platelets or white cells are low, ask your nurse for advice about having sex. Your nurse can help and support with issues affecting your sex life or close relationships.
Even though you are likely to be infertile after the high-dose chemotherapy, there is no guarantee that it will happen. Research suggests that a small number of patients recover fertility after a transplant. It is important to use reliable contraception such as a condom after chemotherapy to avoid pregnancy. This is because the drugs might harm a developing baby. Your doctor or nurse will advise you on this.

Long-term recovery
The length of time it takes for you to fully recover from the transplant is a very individual thing and depends on the type of transplant that you have had. Going back to work and family life can be difficult after focusing on your treatment and it may take time to adjust but most patients are happy with the results of their treatment and are very positive about their future. We have more information on life after treatment.
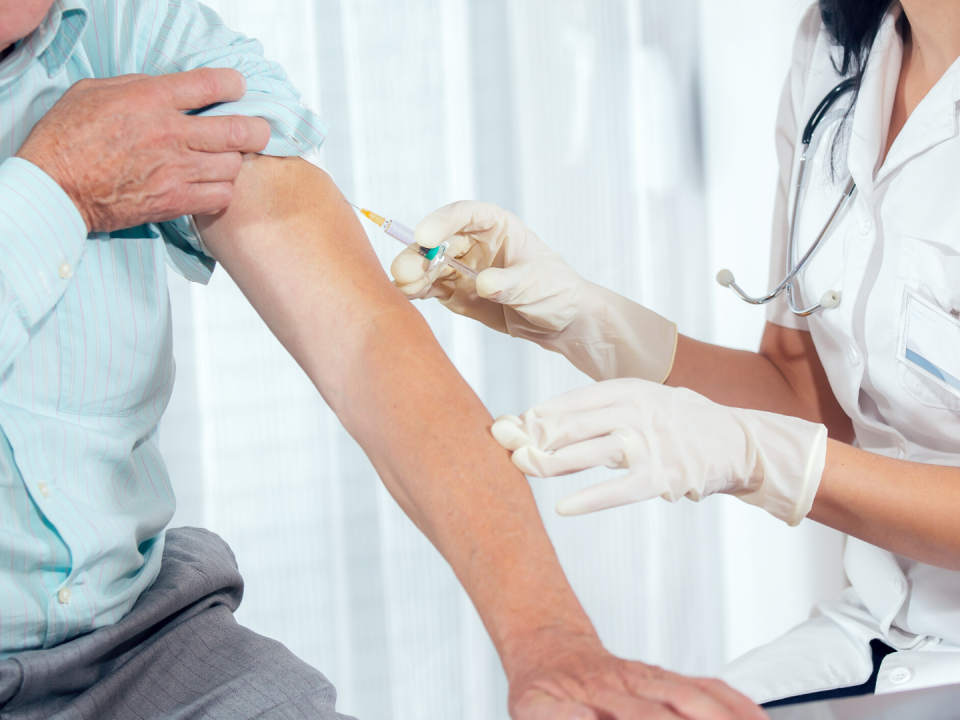
Vaccinations
The transplant means you lose your immunity to all of the diseases that you were vaccinated against as a child so you will need to have them again to get the protection. Your doctor will let you know when you are ready to have your vaccinations. These include measles, mumps, rubella and the non-live polio vaccine. This will usually be after a year or so, when your new immune system should have fully recovered.
Relapse (cancer returning after treatment)
It is possible for the cancer to come back again (relapse) after a stem cell transplant. This is more likely in the first 2 years after transplant, after this time the risk of relapse reduces. If your cancer comes back, your consultant will discuss your treatment options with you, taking into account your medical history and your general health.
For more information
Phone
1800 200 700



