Surgery for muscle-invasive bladder cancer
On this page:
Removing some or all of the bladder
The aim of surgery for muscle invasive bladder cancer is to remove the cancer and the area close to it. Surgery to remove your bladder is called a cystectomy.
If the surgeon removes just part of your bladder, this is called a partial cystectomy.
Usually the whole bladder will be removed, which is called a radical or total cystectomy.
In a radical cystectomy, your surgeon may remove nearby tissues, lymph nodes and organs. In men, the prostate, seminal vesicles and part of the vas deferens and urethra may be removed. In women, the uterus, fallopian tubes, ovaries, and part of the vagina may be removed.
Surgery to help you live without a bladder
If your bladder is removed, you won’t be able to pee in the usual way. Your surgeon will need to find a new way to drain your urine. There are different ways to do this:
- Urostomy (‘your-oss-tommy’)
- Continent urinary diversion
- Bladder reconstruction (neobladder)
Urostomy
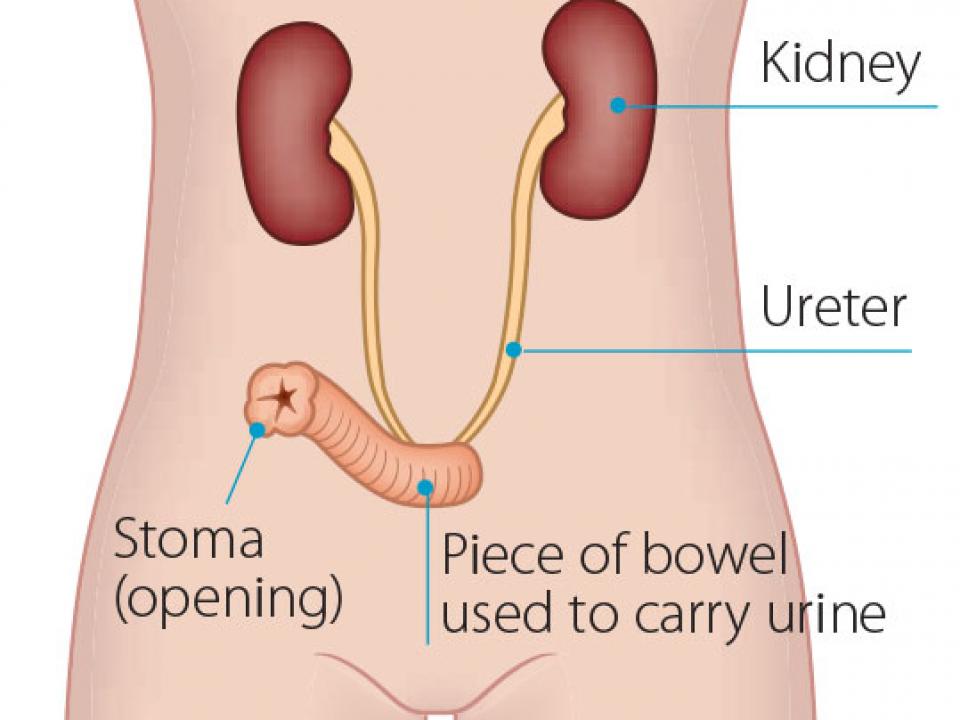
Most patients who have a cystectomy will have a urostomy. Your surgeon uses about 6 inches of your small bowel to make a tube that comes through the surface of your tummy.
Clearing your bowels: You may be asked to follow a special diet for a few days before the surgery or to drink a laxative. This is so that your surgeon can get a clean segment of bowel to make the urostomy.
The two kidney tubes (ureters) will be then be attached to the tube. One end of the passage is closed up with stitches, while the other end is brought through to the surface of your tummy. The open end is called a stoma and looks like the skin inside your cheek. You will need to wear a bag attached to the stoma to collect and drain your urine. A flat, watertight bag is placed over the stoma to collect your urine. It’s kept in place with a special type of glue. The bag will fill with urine, and you will need to empty it regularly. A stoma nurse will show you how to take care of it.

Stoma nurse: The stoma nurse will visit you before surgery to discuss having a stoma. She or he will mark on your skin the best place for the new stoma to be located. She will show you how to take care of it afterwards.
Stents
For the first 7 to 10 days after your urostomy you will have fine plastic tubes called ureteric stents in you ureters. These keep the ureters open and working while you’re healing.
They will usually be removed when you return for your follow-up appointment.

Getting urostomy supplies: When you leave hospital, you will be given some dressings and urostomy bags to last a few days. You will also be given a prescription for more supplies from your pharmacy. Go to the pharmacy to get these as soon as possible. Most pharmacies do not keep them in stock and it may take a few days for supplies to arrive.
Continent urinary diversion
With this type of urinary diversion, you don’t need an external bag to collect your urine. Your surgeon uses a piece of your bowel to make an internal pouch that can store urine inside your tummy. The two kidney tubes (ureters) will be then be attached to it. Urine will drain through the ureters into this pouch.
The internal pouch is connected to your tummy wall by a stoma. Your surgeon will create a one-way valve to keep the urine inside the pouch.
You empty urine from the pouch through the stoma using a thin tube called catheter. You will need to do it about 5 or 6 times a day. A stoma nurse will teach you how to do it. The stoma is covered with a bandage.
Bladder reconstruction
In this type of surgery, instead of making a stoma, the surgeon makes a new pouch out of bowel tissue. The kidneys drain the urine into this pouch. The pouch is then is connected to your urethra.
The pouch (known as a neobladder) stores urine like your bladder did, and you pass urine out through your urethra.
You can empty the pouch by holding your breath and pushing down into your tummy. You will need to do this regularly as you won't know when your bladder is full. Your hospital team will give you more information about this.
Will I get side-effects from surgery?
Surgery to the bladder can affect your bowel and may also affect your sex life. You may also have a urostomy bag, which can take a while to get used to. Read more about the side-effects of muscle-invasive bladder cancer surgery.
For more information
Phone
1800 200 700





